Once again, another accolade contributing to Gardner’s distinction as the “Model City for America” as Heywood Healthcare is featured as a great model for patient safety by the Massachusetts Board of Registration in Medicine. Congratulations, Heywood Healthcare! Copy of above graphic in printable letter size, CLICK HERE.
Heywood Healthcare Featured for Quality and Safety
The Chair Man and the Chair Lady speak of Heywood’s culture of excellence in healthcare in the context of Heywood being featured in the Massachusetts Board of Registration in Medicine’s Spring 2026 Quality and Patient Safety Newsletter. Listen on any device, CLICK PLAY.
Here’s a copy on PDF of the State Newsletter in which Heywood is so prominently featured, CLICK HERE.
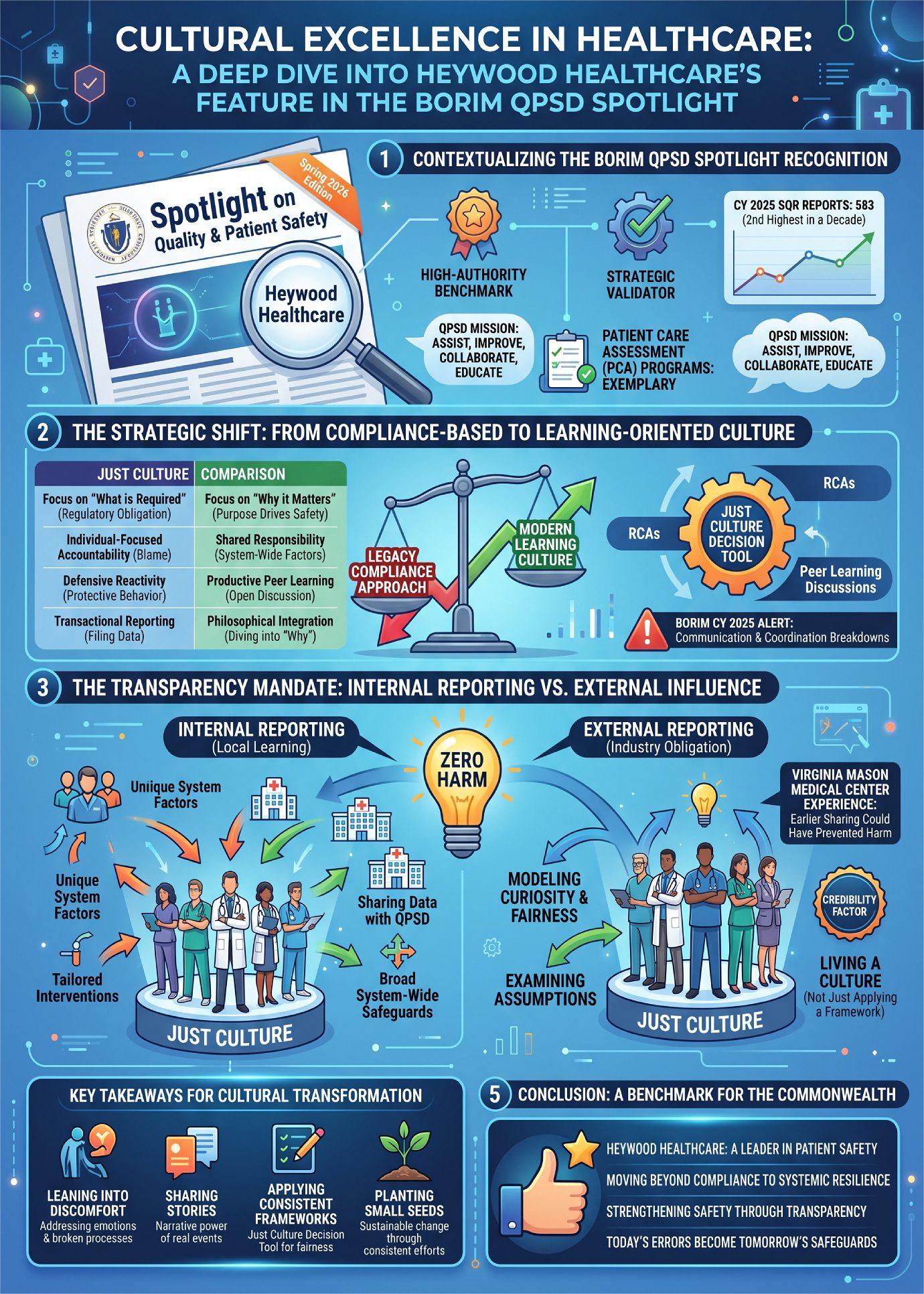
Heywood Healthcare posted: “We’re proud to share that Heywood Healthcare has been featured in the Massachusetts Board of Registration in Medicine’s Spring 2026 Quality and Patient Safety Newsletter! This issue highlights important work across the Commonwealth, including our contribution, “From Compliance to Learning: Strengthening Safety through Transparency.” It reflects our continued commitment to building a strong safety culture, fostering transparency, and learning from every experience to improve patient care.”
The “Spotlight on Quality & Patient Safety,” issued by the Massachusetts Board of Registration in Medicine (BORIM) Quality & Patient Safety Division (QPSD), represents the high-authority benchmark for clinical excellence within the Commonwealth. More on this below.
Purpose of the State Report: This report from the Massachusetts Board of Registration in Medicine examines patient safety data collected throughout 2025 to improve healthcare quality across the state. The findings highlight that while most reported incidents resulted in temporary harm, critical issues remains regarding surgical complications, diagnostic delays, and medication errors. Analysis reveals a concerning demographic disparity, noting that while minority populations often face higher risks, they are frequently underrepresented in voluntary safety reporting. The document also identifies communication breakdowns as a primary driver of adverse events and advocates for increased transparency and safety culture within medical facilities. By sharing these trends and specific case data, the Board aims to foster a collaborative environment where providers can learn from mistakes to prevent future medical errors.
Why Heywood’s Inclusion is so Prestigious
The “Spotlight on Quality & Patient Safety,” issued by the Massachusetts Board of Registration in Medicine (BORIM) Quality & Patient Safety Division (QPSD), represents the high-authority benchmark for clinical excellence within the Commonwealth. For healthcare leadership, a feature in this publication is a significant strategic validator, signaling that an organization’s Patient Care Assessment (PCA) programs—spanning quality assurance, peer review, and risk management—are not merely functional, but exemplary.
The QPSD’s role is to provide the “ground truth” for safety standards, serving as both a regulator and a collaborative partner in clinical improvement.
“QPSD Mission is to assist Massachusetts healthcare facilities in maintaining and improving systems for patient care that are evidence and team-based, sustainable, safe, and inclusive. We achieve this by reviewing data, listening, collaborating, and educating teams in healthcare facilities throughout the state.”
The prestige of Heywood Healthcare’s feature in the Spring 2026 edition is contextualized by a high-stakes, high-volume data landscape. In CY 2025, the QPSD managed 583 Safety & Quality Review (SQR) reports documenting 692 unexpected events. Critically, these 583 reports—which notably exclude aggregate patient falls and pressure injuries—mark the second-highest volume of reporting in nearly a decade, surpassed only by the 589 reports filed in 2019. In an environment of such high clinical volatility, Heywood Healthcare has distinguished itself not just by reporting data, but by providing a strategic blueprint for cultural evolution.
The Heywood Culture of Excellence Revealed in Detail
Heywood Healthcare’s evolution reflects a transition from rigid accountability to a sophisticated model of shared responsibility:
| Legacy Compliance Approach | Modern Learning Culture |
|---|---|
| Focus on “What is Required”: Viewing reporting solely as a regulatory obligation. | Focus on “Why it Matters”: Emphasizing the purpose behind the standard to drive safety. |
| Individual-Focused Accountability: Identifying a person to blame for clinical deviations. | Shared Responsibility: Integrating “Just Culture” to explore system-wide factors. |
| Defensive Reactivity: Protective behavior during event reviews and investigations. | Productive Peer Learning: Open discussions focused on identifying system vulnerabilities. |
| Transactional Reporting: Filing data points to meet state-mandated deadlines. | Philosophical Integration: Diving into the “why” behind the safety philosophy. |
This cultural shift is operationalized through the Just Culture Decision Tool. By integrating this framework into Root Cause Analyses (RCAs) and Peer Learning Discussions, Heywood has successfully neutralized the fear of retribution. This is a direct strategic response to the current clinical climate; as BORIM’s CY 2025 Patient Safety Alert highlights a statewide trend in communication and coordination breakdowns, Heywood’s move to lower defensive barriers serves as a prerequisite for solving the very transparency issues currently challenging the Commonwealth.
Heywood as a Benchmark for the Commonwealth in the “Model City for America”
Heywood Healthcare’s feature in the Spring 2026 Spotlight reinforces its status as a leader in patient safety within Massachusetts. In an era where SQR reporting volumes are at near-historic highs, Heywood’s decision to dive into the “why” behind their safety philosophy distinguishes them from the hundreds of other facilities merely reporting data. They have moved beyond the baseline of compliance to provide a roadmap for true systemic resilience.
Another positive development at Heywood
Life Flight will be landing much closer to the Heywood ER with the new helipad at the hospital in Gardner. The goal is to improve response times and streamline critical patient transfers. In the past, Life Flight has landed at MWCC and the Gardner Municipal Airport. Operational start date will be announced soon.























